Poster Presentation: Educating pathologists in quantitating stromal tumor-infiltrating lymphocytes in breast cancer for artificial intelligence applications
Authors
- Victor Garcia
- Amy Ly
- Roberto Salgado
- Brandon D. Gallas
Abstract
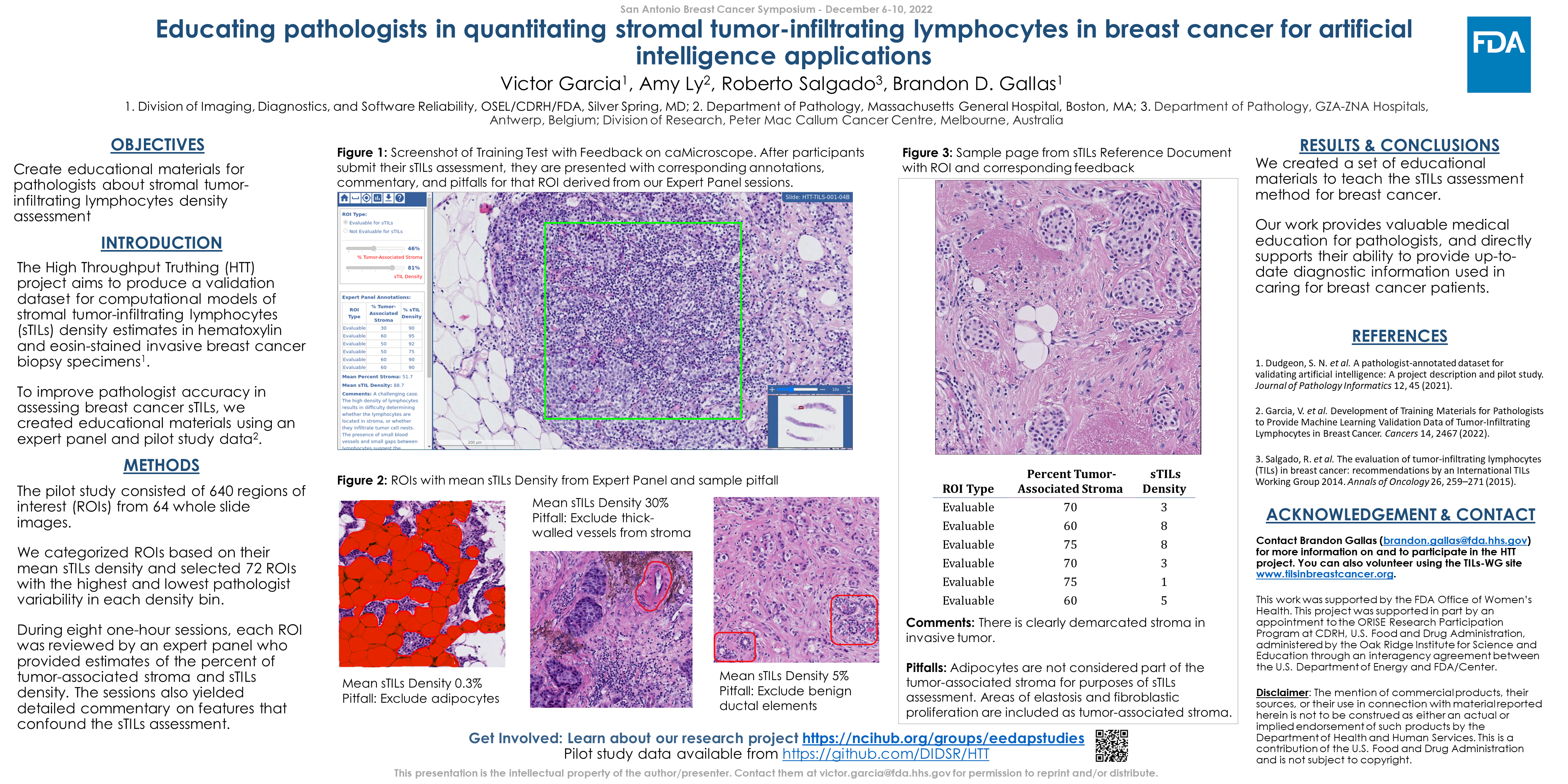
Background: Immune cells in the tumor microenvironment play an important role in cancer development.1 In triple negative breast cancer (TNBC), stromal tumor-infiltrating lymphocytes (sTILs) have been identified as a biomarker with both predictive and prognostic clinical values2. The High Throughput Truthing project collected sTILs density estimates in hematoxylin and eosin stained invasive breast cancer biopsy specimens. The goal of the project is to produce a dataset to validate artificial intelligence and machine learning models3. After collecting annotations from pathologists for a pilot study, we observed a high level of interobserver variability in sTILs density estimates. To improve pathologist accuracy in breast cancer sTILs assessment, we created educational materials using an expert panel and pilot study data.
Method: The pilot study data consisted of 640 unique regions of interest (ROIs) derived from 64 digital whole slide images. We categorized ROIs based on their mean sTILs density as “10% or less”, “11% to 40%”, or “greater than 40%”, and selected 72 unique ROIs from those with the highest and lowest pathologist variability in each density bin. In a series of eight one-hour sessions, each ROI was reviewed in a group setting by at least three members of our expert panel, which consisted of one clinical scientist and seven board-certified pathologists trained in breast cancer sTILs assessment. Experts provided estimates of the percent of tumor-associated stroma and sTILs density, and commentary on features that confound sTILs assessment for each ROI.
Results: We created a set of educational materials to teach the sTILs assessment methodology in breast cancer. These materials include an introduction to the clinical relevance of tumor infiltrating lymphocytes in the breast cancer microenvironment, a tutorial for assessing sTILs according to published guidelines4, and a discussion of specific pitfalls that may be encountered. Expert panel annotations, comments, and pitfalls were used to generate a reference document and interactive tests: one with expert feedback on each ROI and one to determine proficiency.
Conclusions: Educational materials designed by an expert panel will serve as reference materials for learning sTILs assessment in breast cancer. Our work provides valuable continuing medical education for pathologists, and directly supports their ability to provide up-to-date diagnostic information used in caring for breast cancer patients.